Osgood Schlatter Disease (OSD) is a common cause of knee pain in children and young athletes.
It’s traditionally categorized as growing pains yet this label often complicates a swift recovery.
As a Physiotherapist actively trying to better understand and solve OSD, it seems we might be missing something here.
I've come to understand it may be less growing-related and more to do with lower back dysfunction - as weird as that may sound.
So if you have it, or are the parent of someone who does, join with me as we discuss a new perspective on Osgood Schlatter Disease. Let's try to pave the way for better management.
Osgood Schlatter Disease
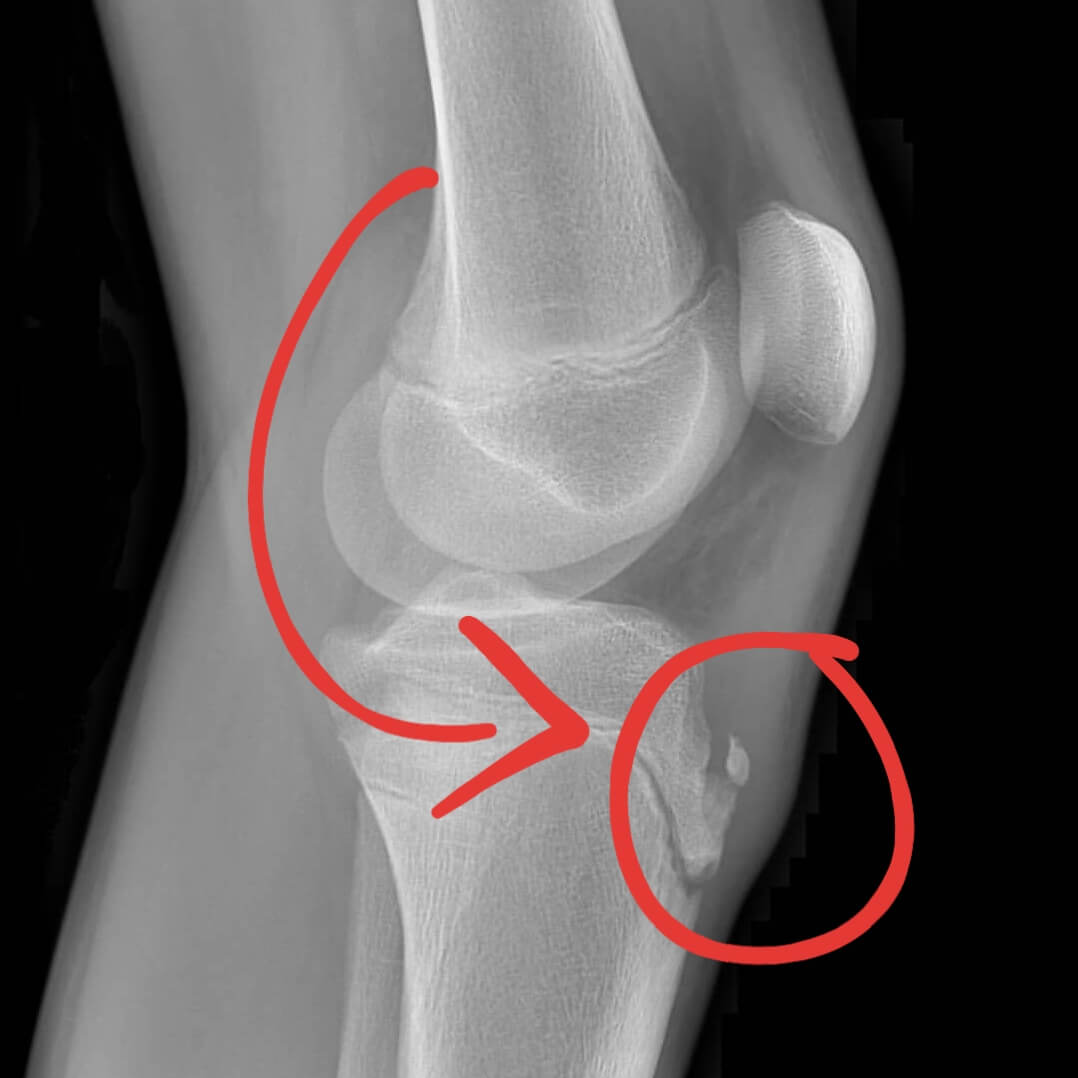
Osgood Schlatter Disease, commonly misinterpreted as Osgood Slaughters Disease, is typified by pain at the front of the knee in adolescents. More specifically, it relates to the stereotypical Osgood Schlatter bump at the top of the shin (seen in the Osgood Schlatter Disease x-ray below).
It was first described by two surgeons - Robert Osgood and Carl Schlatter way back in 1903. And it's still an issue over 100 years later.
Anatomically, it relates to accumulated trauma at the insertion of the Patella tendon to the Tibial Tuberosity. Medically, it can be seen as a traction apophysitis.
When young, this bump is a softer, developing cartilage as opposed to hardened adult bone.

Interestingly, Osgood Schlatter Disease can affect up to 10% of young athletes with up to 30% of those suffering from the condition on both knees.
That's a lot of young, sore knees.
Despite the stereotype, we can still see Osgood Schlatter in adults. But more on this a little later.
It’s also worth reassuring those with OSD the term disease is a little misleading. It’s not actually an illness or sickness and should really be called Osgood Schlatter Dysfunction based on its presentation.
Osgood Schlatter Disease Symptoms
- Knee pain and tenderness
- Observable bump at the top of the shin, under the knee cap
- Pain that worsens with exercise
- Prolonged pain post-exercise
The symptoms vary and so will a person’s ability to tolerate exercise. Some can continue to be active while some cannot.
Osgood Schlatter Disease Cause
As mentioned before, OSD is filed under growing pains. It’s seen as the result of rapidly growing tissue unable to cope with the dynamic demands of exercise and activity.
Activities linked with the dysfunction generally involve running, jumping and landing.
In short, if you're growing and physically active, then you're at risk.
Osgood Schlatter Disease Treatment
Treatment of Osgood Schlatter Disease typically relies on a mix of symptom and activity management.
Here are some traditional treatments:
- R.I.C.E (despite an industry shift in the way we use ice)
- Complete rest or reduction of activity
- Taping
- Bracing
- Various leg strength and mobility exercises
How Does Osgood Schlatter Disease Go Away?
Frustratingly for many, Osgood Schlatter Disease’s link to growing is often used as an excuse for inadequate management.
It’s common to be told the symptoms will go away once you’ve stopped growing. This can be anywhere from 6 months to a number of years depending on when it developed.
But this thinking suggests we don’t fully understand the true cause of OSD. That growing and using your knee (which are normal) are needed to stop for it to get better. And when you’re looking to fix Osgood Schlatter Disease, this isn’t what you want to hear. More on this a little later.
This is particularly relevant when you consider many fully grown adults still have the dysfunction.
Osgood Schlatter Disease in Adults
Osgood Schlatter Disease can still affect those who've stopped growing. I don’t have the statistics, but I’ve personally treated a number of fully grown adults with symptomatic Osgood Schlatter Disease - despite being in their 20s and 30s.
This isn't to say they have developed the condition as adults, but their symptoms are certainly still present.
Adult Osgood Schlatter Disease is part of the reason why I’d like to challenge a few long-held beliefs regarding the cause of OSD.
Things don’t entirely make sense all things considered. And I think we might be missing the foundation of its origin.
What Could We Be Missing?
To be fair, traditional thinking around Osgood Schlatter Disease does make sense on a number of levels. If a growing body meets rigorous activity, it's easy to see how some underdeveloped areas can be vulnerable to dysfunction.
But considering at least 70% of OSD cases are one-sided, surely this points to something broader at play?
I mean, if someone's knee pain is the result of growing, yet is only on the one side, does that mean they’re growing asymmetrically?
Obviously not.
There has to be something else we’re aren’t seeing.
Let me explain further.
Why Osgood Schlatter Disease Isn't Growing-Related
Before we get into specifics, let's discuss why Osgood Schlatter disease shouldn't be considered growing-related:
- Growing is normal by definition
- Pain is considered abnormal
- Logically we expect growth to be symmetrical. Yet the majority of those with Osgood Schlatter Disease have pain on one side, or pain greater on one side
- Exercise and activity are also normal
With these factors in mind, why should two normal things - growing and movement - conspire to give children and teenagers knee pain? Unless we're missing something...
From what I’ve come to understand clinically, there might be a perfectly good explanation for all of this.
My Experience With Osgood Schlatter Disease
Full disclosure: I had Osgood Schlatter Disease as a teenager, and it was crappy.
As a junior AFL footballer (for those outside Australia feel free to look it up, it's awesome) I had pain on both sides (left worse than right) for almost three years.
It impacted my ability to run, jump, kick a ball, surf, bike ride and generally be active.
When seeking treatment I was given thigh-strength exercises, various leg stretches, shown how to tape it and off I went.
Disappointingly, I was also told to wait it out. That it'd get better once I finished growing.
Looking back now that I've been a Physical Therapist for well over a decade, I'm left a little frustrated at what could have been.
I know now that my specific prognosis should have been closer to 2-3 weeks, not most of my mid-late teens.
I still have the Osgood Schlatter Disease bumps to show for it, perhaps unnecessarily.
Is There a Better Explanation Than Growing Pains?
As mentioned above, it's important to acknowledge that our current thinking does make sense. Growth plus activity could logically create pain and dysfunction on its own.
Yes OSD is still an overload and irritation of the knee.
Yes, the bump at the top of the shin is susceptible with young athletes as it's yet to become rock-solid, permanent adult bone.
But there’s one factor that seems integral to the onset and persistence of Osgood Schlatter Disease.
It's not growing.
It's not activity either.
Instead, it's potentially a small section of the lower back.
What I'm Finding Clinically
Clinically I'm finding that stiffness at the base of the ribcage/top of the lumbar spine may mechanically set the knee up to fail.
Anatomically, this is approximately T10 - L2 for the nerds.

It’s worth noting that I’m not talking pain here, just stiffness. Something you need to directly look for to find.
This area is important as it has nerves that supply and control the thigh and knee.
If the lower back stiffens there can be a chain reaction of neural and muscular tightness to related areas.
The result? Greater resting tension through the quadriceps, patella tendon and tibial tuberosity (shin bump).
This may cause young athletes to load a vulnerable area poorly.
Furthermore, those suffering from Osgood Schlatter Disease often have their low back stiffness on the same side as their knee pain.
This may indicate why the majority of young athletes have one-sided pain or greater symptoms on one side.
Like my patients, my back was also stiff, more so on the left than right as per my symptoms. I just had no reason to connect the dots.
If interested, I've covered an eerily similar idea in an in-depth article on knee tendonitis. The way I see it, Osgood Schlatter Disease is potentially the adolescent version of adult knee tendonitis.
New Approach to Osgood Schlatter Disease Treatment
I still highly support the way we treat Osgood Schlatter Disease.
- De-irritate the knee with relative rest and soft-tissue massage
- Work hard on the mobility of your calves, hips, quads and hamstrings
- Work hard on the strength of your calves, hips, quads and hamstrings
- Consider the use of an Osgood Schlatter Disease brace that sits across the patella tendon and helps disperse the load
At this point, it's also worth noting we should reconsider the use of ice to treat any injury let alone the symptoms of Osgood Schlatter Disease.
With this being said, just do yourself a favor and have your lower back assessed. Have someone look beyond your knee pain and focus on finding that potentially stiff or restricted low back tissue. From my experience, it's highly likely to be there.
Thankfully there are also some things you can try at home.
Lower Back Exercise For Osgood Schlatter Disease
Take a foam roller, lacrosse ball or even a rolled-up towel and go hunting for yourself.
When thinking Osgood Schlatter and foam roller, we typically think legs - in particular the quads and calves. But it's brilliant for freeing up the spine as well.
Lie down and let your tool of choice gently press into your stiff and tight areas. Try not to roll around, instead stay still, relax and let your tissue give slowly.
One side of your spine may be stiffer so make sure you check both. Also, make sure you can breathe comfortably and deeply throughout.
Spend a few minutes on each stiff or tender spot and then move on.

Respect Good Spinal Shapes
No back-specific discussion is complete without mentioning sitting posture. Good postures and positions are crucial for a healthy functioning spine.
Obviously any sitting is a challenge for the body over time, but it's important to optimize your posture where possible.

When looking at those with OSD, it's common to see a slouchy hinge created in the lower third of the spine (left) when sitting.
This hinge is by no means Osgood Schlatter-specific but it's an obvious sign of a low back highly likely to be dysfunctional. Notice a huge difference on the right when I sit upright. Remember, I suffered from OSD as a kid as well.
If you're a parent try and watch how your son or daughter sits at home on the couch, at the dinner table, in the car or even up in bed at night. From what I'm finding clinically, they may not be model citizens - unintentionally of course.
It's a vitally important component to try and improve. If you can, the hidden back stiffness should not return. But they might if the less than perfect habit is left unchecked.
Core Strength Is Still Important
Core strength is still really important for those with Osgood Schlatter Disease.
Like many knee injuries, OSD benefits from a strong and stable trunk and pelvis. This allows for better loading and control at the knee itself.
The simplest way to start improving core strength in adolescents is with the plank and its many variations. Aim to be able to hold it for a few minutes. Alternatively, try 4-5 sets of 30-second holds. We just want to feel fatigued, so how you approach something like this is up to you.
Consider lifting an arm or leg off the ground to make it harder. Both if you want it harder again. There are side planks, planks with hands and feet on balls, rollouts and many more.
Boring, but all basic and very effective.
Similarly, improved core strength makes it easier to sit in more upright positions. It still takes a conscious effort (sitting is a passive shape after all) but it becomes far easier to maintain with a stronger trunk to work with.
Improved core strength can help you recover that little bit faster from OSD. It will also help to improve the factors that set young knees up to fail in the first place.
Frequently Asked Questions
The symptoms of Osgood Schlatter Disease tend go away once the Tibial Tuberosity (classic knee bump) is better loaded. The general consensus is this happens once you stop growing. But technically this isn't the case - there are adults with OSD.
The shin bump does naturally morph from softer, adolescent bone to harder, adult bone with age, but this isn't the key ingredient it's made out to be. Improving the way you load the knee is. Once you have improved the function of your lower back (as per this article), loosened up your thigh and hip muscles and improved your core and gluteal strength the symptoms should truly start to settle. It shouldn't matter how old you are.
It's worth noting that the classic bump associated with Osgood Schlatter Disease does not often change. Once it becomes hardened bone it's often there forever - without causing any additional issues.
The classic Osgood Schlatter bump is the body's way of trying to reinforce against poor loading of the Tibial Tuberosity. The tuberosity begins as softer bone and hardens as we mature. Altered loading forces the body to lay down more bone than usual to compensate leaving the raised Osgood Schlatter bump behind.
The bump associated with Osgood Schlatter Disease is often permanent and does not go away. In the process of developing OSD, the body can lay down more bone to buffer the change in loading. Once the symptoms have gone the bump remains a cosmetic concern rather than a functional one.
Interestingly, Osgood Schlatter Disease is seen as 'Growing Pains', yet can still effect many adults. This is because OSD should be thought of as a knee loading issue, not one solely vulnerable to growth. If an adult doesn't restore normal loading to the knee it can still present a problem long after growing has ceased. Adult Osgood Schlatter Disease can be associated with or a precursor to knee tendonitis.
The short answer is no. Clearly there may be extreme cases where surgery is the last resort, but most cases of OSD are managed conservatively with great success.
Surgery can remove the bump associated with Osgood Schlatter Disease however this is rarely necessary. Furthermore, any surgery to adolescent growth plates has the potential to cause ongoing knee dysfunction later in life. While an understandable option for those seriously struggling, surgery should rarely be an option if OSD is managed appropriately.
Short answer, no. Running may irritate Osgood Schlatter Disease however it is considered a self-limiting condition and not overly serious. Like any musculoskeletal issue you must respect your symptoms and manage activity levels appropriately. It's fine to continue to be active with the help of tape and/or a brace if that makes you happy. But make sure you are also seeing progress in your rehab behind the scenes. If you are not getting stronger and more mobile in the right areas then you can't expect OSD to eventually go away.
If you are continuing to be active but your pain is not improving, or even getting worse, then it may be time to heavily consider a period of relative rest. Don't stop all activity - just the things you find irritate the knee. Once your rehab has progressed further gradually re-introduce any aggravating activities.
A lateral x-ray may show the superficial Osgood Schlatter bump and potential bone fragmentation at the Tibial Tuberosity.
No, Osgood Schlatter Disease is no more dangerous than any other common musculoskeletal dysfunction. The disease label can sometimes confuse those when diagnosed, however OSD should not be confused with medically based diseases.
Conclusion
Despite carrying the label of growing pains Osgood Schlatter Disease might be anything but - particularly when considering the many adults with the condition.
The asymmetrical nature of most people's symptoms might suggest otherwise. Those with adult Osgood Schlatter disease may also disagree.
From what I've come to understand clinically, the mid-low back may be the underlying culprit here. Mechanical dysfunction may create a chain reaction of events ending in a vulnerable part of the knee becoming overloaded and irritated with use.
Consider adding some back specific mobility to your Osgood Schlatter Disease exercise routine. Similarly, please heavily consider how you position your back throughout the day. It may just be the foundation of your dysfunction.
Encouragingly, don't wait until you finish growing before expecting change (like I had to). You deserve to see change regardless.
What has been your experience with Osgood Schlatter Disease? What are you doing to get better?


3 comments
Hi Laura! Glad to hear you may have found something helpful! Absolutely let me know how you guys go!
I’m so grateful to have found your website and information. My 14 year old son suffers so much and we are in a really tough time with the OS issue . His knots are getting bigger each day . He’s in constant pain – we’ve taken him to orthopedic doctors, growth specialists, sports medicine doctors and we get told the same thing … it will go away .. in the mean time rest and ice and stretch . My son’s sports are his life , his passion and I think stopping for a year or two would hurt him more in the long run that dealing with these knots his whole life . The problem is , he is a slow grower . He’s super short and is having late onset growth… so we are literally just waiting for a miracle .. some doctors say he won’t finish growing until he’s a senior in high school .. so he has to wait and live like this for four years . I am always searching for answers and solutions and when your video popped up and mentioned lower back pain , it was like a lightbulb for me . My son , says his power back hurts all the time too . The doctors said that was a growth issue as well . But , I’m so , so hopeful right now that if we take him to a chiropractor or a deep tissue masseuse, we can work on the lower back and relieve the load on the knee( as I learned from your advice ). It makes so much more sense to me than the growth issue . For once on a year almost , I have hope and I thank you for that . I’d love to keep you updated on my son’s progress and if this works for him . If it does , then you will have changed his life and I would want that for any other kid’s suffering with this condition. I hope you receive this message ! Please email me if there is anything else you recommend. Thank you so much .
Laura
Ongoing health issues with my friend Carolyn Brown-Hodnett-Brown now almost 69 years old. Osgood-Schlatte