
Neck-Related Headaches: A Physio's Guide to Understanding and Relief
By Grant Frost · Physiotherapist
•
Last clinically reviewed: 25 March 2026
Key insights: 60-second read
- Neck dysfunction may cause or contribute to most headaches – The upper neck (C1-C3) has strong neural connections to the head and face.
- Symptoms can be widespread – Pain may be felt behind the eyes, base of skull, temples, forehead, sinuses, ears, jaw, or teeth.
- Posture is a key driver – Prolonged looking down (phone, computer) overloads neck tissues, making headaches the "last straw."
- Self-treatment works – Neck mobilisation with a ball, postural correction, and deep breathing can provide significant relief.
Do you suffer from headaches? More importantly, do you feel like they are under control? If you experience regular headaches, you will know how debilitating they can be, creating a significant handbrake on your capacity to think, be social, and feel happy.
From my experience as a physiotherapist, I have found that neck dysfunction may cause, or at least heavily contribute to, the majority of headaches people experience. This is not to say all headaches are neck-related, but it suggests there is a strong chance you can do something about them.
If you are looking to better understand your headaches and how to conquer them, this professional advice will help you identify the signs and find effective relief.
On this page
1. Understanding Headaches: Primary vs. Secondary
A headache can be an unexpected ache, pain, or tension anywhere on the face, head, or top of the neck. Staggeringly, almost half the adult population has had a headache within the last year.
Headaches are broadly categorised into two types depending on their source:
- Primary Headaches: The headache itself is the primary medical condition.
- Secondary Headaches: The headache is a symptom of another underlying issue.
Primary Headaches
These are the most common types of headaches and include:
- Tension Headaches: Often felt as tightness and pressure around the forehead and base of the skull. They can appear on one or both sides and are frequently linked to stress.
- Migraines: Typically a one-sided, throbbing pain that may be associated with 'Aura' - reversible neurological symptoms like visual disturbances. Severe tension headaches are sometimes confused with migraines.
- Cluster Headaches: Intense, cyclical attacks of pain, usually behind one eye. These are among the most severe types of headaches.
Secondary Headaches
These are symptoms of an underlying condition. Headaches associated with structural neck dysfunction (known as cervicogenic headaches), infections, head trauma, and even hangovers or 'ice-cream' headaches fall into this category.
The Neck-Headache Connection
Despite these classifications, neck dysfunction is a common factor in many headache types. The following information will help you determine if your neck is causing or influencing your headaches.
2. Symptoms of a Neck-Related Headache
Clinically, neck-related headaches can present in various ways, from a vague, hard-to-localise ache to a sharper, more specific pain. The pain can be referred to many areas, often on one side but sometimes both:
- Behind the eyes
- The base of the skull
- Temples and forehead
- Top of the head
- Sinuses, ear, jaw, or even the teeth
Associated symptoms can also include:
- Pressure or tightness
- Dizziness and light-headedness
- Tinnitus (ringing in the ears)
- Mild loss of balance, nausea, and brain fog
- Light sensitivity, blurred vision, or eyelid twitching
- The sensation of a blocked sinus or skin sensitivity
Important: Many of these symptoms can relate to other medical issues. It is crucial to consult a healthcare professional for an accurate diagnosis.
3. Red Flags: Symptoms of Serious Headaches
While most headaches are not sinister, you must seek immediate medical assistance if you experience any of the following:
- A sudden, severe 'thunderclap' headache
- Slurred speech, confusion, or memory loss
- Severe loss of balance or trouble moving your limbs
- Seizures, vomiting, or a fever
These symptoms may indicate a more serious condition, like a brain aneurysm or tumour and should not be ignored.
4. What Causes Neck-Related Headaches?
Simply put, many headaches are referred from stiff, overloaded, and irritated tissues in the upper neck and base of the skull. This connection is often easy to identify; pressing on areas of joint stiffness or muscle tightness in the upper neck can reproduce headache symptoms. Conversely, successfully treating these areas can reduce the symptoms.
The Role of the Upper Neck
The upper neck (the Occiput/C1, C2, and C3 spinal levels) has strong neural connections to the head and face. When these areas become dysfunctional, they can refer pain. These connections are known as dermatomes.
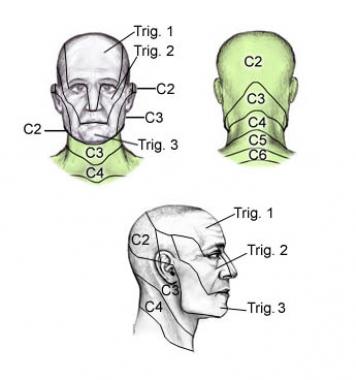
Complicating diagnosis is the fact that you may have no awareness of neck dysfunction. The neck itself may not feel stiff or painful, which is why it is crucial to consider the neck as a potential source.
The Impact of Posture
To understand the cause, we must ask why healthy neck tissue becomes stiff and overloaded. Headaches are often the 'last straw' after prolonged stress on the neck from daily activities such as:
- Using your phone or laptop
- Working at a computer or doing schoolwork
- Reading, watching TV, or playing an instrument
- Cooking and cleaning
These activities often involve looking down or holding the neck in a sustained, less-than-ideal position for hours each day. Over time, this creeps closer to your tissue's pain threshold until a headache is triggered.
5. Common Triggers for Neck-Related Headaches
Common triggers like stress, lack of sleep, alcohol, or certain foods may not be the root cause. Instead, they can expose underlying neck dysfunction that is already present. By improving the health and function of your neck, these triggers often lose their power to cause a headache.
6. The Role of Stress in Headaches
Stress alone is unlikely to cause a headache, but it significantly influences your pain experience. Stress lowers your pain threshold and heightens your nervous system's perception of threat, which can amplify and prolong headache symptoms. Managing stress is, therefore, a key part of treatment.
7. How to Treat Neck-Related Headaches
Professional treatment from a physiotherapist may include massage, joint mobilisation, strength training, and postural correction. However, there are several effective techniques you can try at home.
1. Self-Neck Mobilisation with a Ball
This is one of the most effective ways to release tension in the upper neck.

How to Self-Mobilise Your Neck
Time needed: 10 minutes
- Lie on your back on the floor with a lacrosse ball, tennis ball, or massage ball.
- Gently position the ball under one side of your upper neck, just below the skull.
- Relax your head and let the ball press into tight, stiff, or tender areas. Pay attention to any spots that reproduce your headache symptoms.
- Spend time on the stiffest areas, then move to the next spot. Compare both sides.
This can be done preemptively or during a headache to help reduce symptoms.
2. Postural Correction
Mobilising the neck provides quick relief, but correcting your posture offers a long-term solution.
Aim for a posture where your chin is not poking forward, your head is not tilted, and you are looking straight ahead. Improve your environment by:
- Raising your laptop or computer screen to eye level.
- Holding your phone higher, or lying on your side to use it.
- Adjusting your car's rearview mirror to encourage an upright sitting position.
3. Hot/Cold Contrast Showers
Contrasting temperatures can help down-regulate a hypersensitive nervous system. Try alternating between hot and cold water for 30-60 seconds each during your shower to help short-circuit headache pain.
4. Deep Breathing
Techniques like Box Breathing can cue your nervous system to relax. Inhale for 4 seconds, hold for 4, exhale for 4, and hold for 4. A few cycles can often shift your symptoms.
Conclusion
While there are many types of headaches, a significant number are related to neck dysfunction. A thorough assessment and treatment of the upper neck can often account for many common symptoms. For lasting relief, combine self-treatment techniques like using a lacrosse ball with a conscious effort to improve your everyday posture.
If you or someone you know struggles with headaches, it is worth investigating the neck. You may be pleasantly surprised by the relief you can find.
Are your headaches neck-related? Let me know how you are managing your symptoms below in the comments.
I genuinely hope this article offers a fresh perspective - or at least one useful takeaway. If you have a different issue, or simply want to learn more about how your body moves, head over to the Your Wellness Nerd YouTube channel. Subscribe if you feel inclined, and let me know in the comments what you'd like me to cover next.
– Grant
Frequently Asked Questions
What does a neck-related headache feel like?
It often presents as a vague, non-specific head or facial pain, typically on one side. The symptoms can usually be influenced by pressing on specific tissues at the top of the neck.
What causes a neck-related headache?
They are usually caused by overload and irritation of the joints and muscles in the upper neck, often due to prolonged poor postures like looking down at a phone.
Where can you feel neck-related headaches?
Pain can be referred to many areas, including behind the eyes, the base of the skull, temples, forehead, top of the head, sinuses, ears, jaw, and teeth.
Can tight neck muscles cause headaches?
Yes, but it is important to understand that both tight muscles and headaches are usually a consequence of deeper neck joint stiffness and overload.
One profound insight from this post
"Headaches are often the 'last straw' after prolonged stress on the neck from daily activities like looking down at your phone. By improving neck function, you can reduce their power."
Living With Persistent Pain?
If your pain has lasted longer than expected, feels disproportionate to injury, or hasn't responded to standard treatment, you may benefit from a broader approach. Learn more about our neck pain physiotherapy services in Port Macquarie.
If this resonated with you, you may also find these interesting:
Related posts

This Neck Mobility Exercise Target Joints AND Muscles
Physiotherapist-guided neck mobility exercise using PNF contract-relax to release both joint stiffness and soft tissu...

Is Your First Rib Actually Depressed? Why Posture is Key to Lasting Relief
Struggling with an elevated first rib? Learn why your sitting posture may be the real cause and how a simple ball mob...

